Stabilize. Sustain.
System Build.
CMHO’s 2024 Pre-Budget Submission
Our 2024 Ontario Budget Recommendations
Before the pandemic, 28,000 children and youth were on wait lists for community-based mental health care, with some waiting upwards of two years. Decades of chronic underfunding, shortages of mental health professionals, and a crisis retaining them in the community sector, combined with the toll of the pandemic and rising needs, have created a dire situation for Ontario families. These gaps in care are even more significant for Northern communities, rural and remote communities, and equity-deserving groups. For the 2024 Ontario Budget, we are asking the government to continue to partner with us on our strategy to invest $140 million over four years to stabilize, sustain, and system build in community child and youth mental health so that every infant, child, youth, and family in Ontario has timely and equitable access to high-quality mental health services.
Our kids and families can’t wait.
Before the pandemic, approximately
children and youth with significant mental health needs received no treatment at all.
Sector Challenges
The crisis in child and youth mental health has reached a breaking point. With the increased prevalence of mental health challenges amongst children and youth, demand for services continues to rise. Notwithstanding targeted recent investments, decades of underfunding have resulted in a system unable to meet needs across the province, with families too often turning to hospitals in crisis. At the same time, the community child and youth mental health sector is facing a health human resources crisis, similar to the rest of the healthcare system.
Sector Challenge: Rising Prevalence, Demand, and Hospitalizations
A recent report from the Conference Board of Canada shows a decline in the number of young people reporting excellent or very good mental health over the past two decades. The use of healthcare services by children and youth for anxiety and mood disorders has significantly increased over the past decade.
In 2022, hospital data from the Canadian Institute for Health Information (CIHI) showed that over 1 in 4 hospitalizations (27%) for children and youth were for mental health conditions.
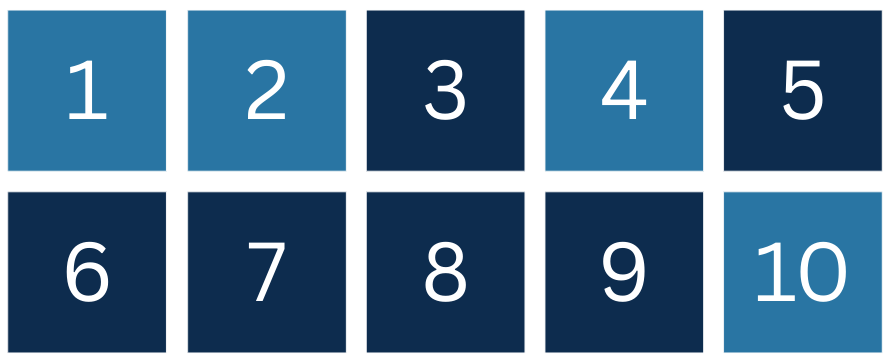
Of the top 10 reasons children and youth ages 5 to 17 were hospitalized, mental health issues took the first, second, fourth, and tenth spots.
Among these needs, we saw and continue to see significant increases in serious mental health concerns such as eating disorders, self-harm, schizophrenia, and substance use.

Northern regions experienced double the rates of hospital utilization compared to the provincial average.
Sector Challenge: Long Wait Times and Service Gaps, Particularly for Equity-Deserving
Groups
Before the pandemic, 28,000 children and youth were on wait lists for community-based mental health care. A further 200,000 children and youth with significant mental health needs received no treatment at all. This is because in some communities, especially Northern, rural, and remote areas, and for some populations, for example, transitional-aged youth and those with concurrent needs such as addictions or autism, the treatments and supports that children, youth, and families need do not exist at all.
There are significant barriers to accessing care for racialized and marginalized populations who struggle to find treatment that is culturally appropriate, identity-affirming, and responsive to their experiences and intersecting needs. At the same time, Black, Indigenous, and racialized youth and those navigating their sexual orientation and gender identity have the highest rates of anxiety and depression.
Sector Challenge: Health Human Resources Shortage
At the same time, there is a health human resources crisis in the community mental health and addictions sector. Agencies have vacancy rates as high as 30% and high turnover rates of 20%. Community child and youth mental health centres struggle to recruit and retain the specialized mental health professionals needed to provide critical treatment and supports to families. The leading cause for this is significant wage gaps with other sectors.

For social worker positions, staff in the community child and youth mental health sector make 20% to 50% less than social workers in the education and hospital sectors.
Stabilize. Sustain. System Build.
The Ontario government has heard the urgent calls of youth and families and has made historic investments in child and youth mental health this past year. However, last year’s base funding increase for Ministry of Health community mental health and addictions agencies primarily mitigated further crises and has helped to keep doors open in the face of rising demand and acuity of need. This is why, for the 2024 Budget, we are asking the Government of Ontario to invest $35 million and commit to a stable, multi-year funding plan so that together, we can:
STABILIZE
Ensure stability for infants, children, youth, and families by closing wage gaps between community child and youth mental health and the hospital and education sectors, so there is capacity to meet mental health needs across Ontario’s communities.
Key recommendations
We recommend that the government stabilize the community child and youth mental health sector now by:
1. Closing the wage gap: Address the wage disparities that exist between community mental health and addictions and other sectors that employ mental health professionals by meaningfully committing to closing the wage gap. This recommendation is part of a broader call with our community health sector partners to close the wage gap facing community-based providers.
2. Removing barriers: Prevent fragmented approaches in funding and policy and put targeted strategies and incentives in place to support and build the workforce in community child and youth mental health.
3. Targeting needs for specific populations: Enable targeted approaches within the integrated system of care supporting the mental health and well-being of infants, children, youth, and youth in the justice system.

SUSTAIN
Start by developing a Workforce Strategy to create a sustainable and responsive community child and youth mental health sector, able to meet the growing demand for services while taking much-needed pressure off hospitals, schools and primary care.
Key recommendations
We recommend that the government enable a sustainable and responsive community child and youth mental health sector by:
1. Developing a Workforce Strategy: Focus on recruitment and retention strategies that attract mental health professionals and prevent turnover into other service systems.
2. Addressing service gaps: Ensure timely access and service availability in child and youth mental health across Ontario’s regions and address operational pressures and infrastructure needs by investing in capital improvements.
3. Reducing wait times: Addressing wait times enables capacity-building in the sector, including the scaling and development of culturally relevant services and programs, and at the same time, takes pressure off other parts of the healthcare system so families don’t turn to emergency departments in crisis.

SYSTEM BUILD
Maximize the impact of all new investments by partnering to build system data and quality improvements and to provide timely and equitable access to services and treatment for all families.
Key recommendations
We recommend that the government prioritize provincial system-building initiatives that advance:
1. Equity: Support the development of a Provincial Equity Strategy for the child and youth mental health sector in recognition of the significant influence of the social determinants of health on mental health outcomes for equity-deserving communities.
2. Quality: Support the development of a Data Strategy by ensuring that data is consistently available, collected, and evaluated across child and youth mental health to support the best possible mental health outcomes for children, youth, and families.
3. Access: Within an integrated systems of care approach, scale successful and innovative models of treatment that enable system capacity building and impact in the community while embedding youth and family voice, addressing service system gaps, and enabling better pathways to care.
Envisioning a Brighter Future
New investments in community-based child and youth mental health centres are urgently needed to begin to close the pay gap and keep the staff we have in order to expand specialized services and treatment.
The children and youth of today who do not get the help they need become the adults of tomorrow who are more likely to struggle with addictions, mental health issues, and undiagnosed disabilities. They can go on to have challenges with long-term employment, housing, justice, and economic needs. Every window where we can intervene early—whether as an infant, child, or young person—is a chance to change a child’s entire life for the better.
The Ontario government has shown its commitment to child and youth mental health this past year and now is the time to continue on that path. Our kids and families can’t wait.
